Inositol, PCOS and Why a Dietitian Matters
Living with PCOS can feel confusing and unfair. Inositol is one tool that can help. It supports hormones, cycles and insulin, but it works best when paired with smart nutrition. That is where a PCOS‑skilled dietitian becomes vital, especially when you factor in findings from PCOS‑specific inositol research.
This article explains:
- How inositol may support PCOS symptoms
- Why diet and lifestyle change still do the “heavy lifting”
- How an Accredited Practising Dietitian for PCOS can safely guide you, including through our broader PCOS nutrition services
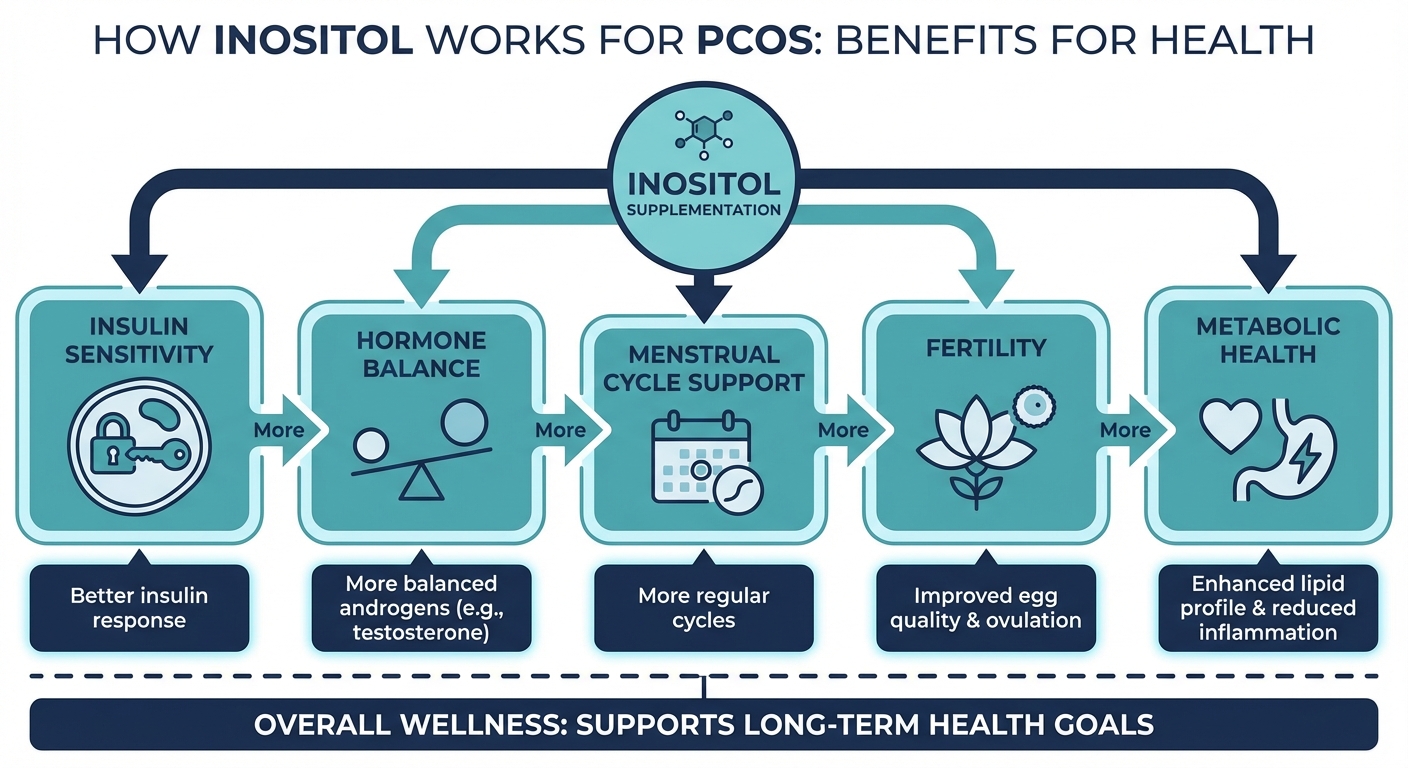
Clinical Benefits of Inositol for PCOS
Inositol is a vitamin‑like compound that helps your cells respond to insulin, with multiple clinical trials and reviews, including a large meta‑analysis of women with PCOS, showing its impact on insulin signalling. In PCOS, that pathway often works poorly, making insulin levels climb and hormones unstable.
- Better insulin sensitivity: Myo‑inositol and D‑chiro‑inositol can lower fasting insulin and improve blood sugar control in many women with PCOS, as demonstrated in controlled trials summarised by reproductive endocrinology research.
- Hormone balance: Over time, inositol may raise sex hormone–binding globulin (SHBG) and reduce androgens, which can calm symptoms like acne and excess hair, a pattern also reported in recent endocrine journal data.
- Cycle and ovulation support: Inositol helps eggs mature properly and can improve ovulation rates and pregnancy chances, especially when started months before trying to conceive.
- Metabolic and heart health: Studies show modest drops in LDL (“bad”) cholesterol and triglycerides, and small weight changes when inositol is combined with lifestyle change.
- Alternative or partner to metformin: For some people, inositol gives similar insulin and fertility benefits to metformin, often with fewer gut side effects, which aligns with safety summaries like the Cleveland Clinic review of inositol.
- Generally well tolerated: Research suggests long‑term use is usually safe, but it should still be used under health professional guidance, and real‑world experiences in PCOS cohorts are described in trials such as a prospective clinical study of myo‑inositol in PCOS.
Inositol is not a magic fix. Think of it as one useful piece in a larger PCOS plan, not the whole plan.
For personalised advice, an AusClin dietitian service can help you decide if inositol is suitable alongside your medical care, and a dedicated PCOS dietitian can integrate it with your broader treatment plan.
Why Work With a Dietitian When Using Inositol for PCOS?
Most PCOS trials with inositol also include structured nutrition and exercise changes, and this combined approach underpins many of the outcomes reported in randomised controlled trials. When people try the supplement alone, results are often weaker.
- Build the right eating pattern: A PCOS dietitian can tailor a lower‑GI or anti‑inflammatory style plan that smooths blood sugar rises and supports ovulation.
- Support sustainable weight change: Even a 5–10% weight reduction can restart periods for some women. That usually needs more than a supplement—it needs habits you can keep, which our structured PCOS nutrition programs focus on.
- Time inositol with food: How and when you take inositol relative to meals can influence symptoms like post‑meal sugar spikes.
- Monitor safety and progress: A dietitian can work with your GP to track cholesterol, HbA1c, liver markers and cycle patterns over time.
- Adjust for different PCOS types: People in larger bodies may see bigger insulin shifts from inositol, while lean PCOS often needs very targeted nutrition and exercise to shift hormones.
- Reduce overwhelm: PCOS brings a lot of noise—supplements, diets, social media claims. A qualified dietitian filters the evidence and builds a clear, step‑by‑step plan.
Our team provides evidence‑based telehealth dietitian consults across Australia, so you can access PCOS support wherever you live, including comprehensive PCOS nutrition counselling from home.
Key Takeaway
Inositol can genuinely support insulin, hormones and fertility in PCOS—but it works best inside a bigger picture. Partner it with an experienced PCOS dietitian, and you turn a simple supplement into part of a structured, long‑term plan for better cycles, health and quality of life, especially when guided by an Accredited Practising Dietitian for PCOS who understands the latest inositol research.
Frequently Asked Questions
Is inositol or metformin better for treating PCOS?
Neither inositol nor metformin is universally “better” for PCOS; they work in similar pathways but suit different people. Metformin is a prescription drug with strong evidence for insulin resistance and diabetes prevention, but it can cause gut side effects. Inositol (usually myo‑inositol with or without D‑chiro‑inositol) can offer comparable benefits for insulin, ovulation and hormone balance in many women, often with fewer side effects. A PCOS‑skilled dietitian at AusClin can help you and your doctor decide which option, or combination, fits your symptoms, goals and medical history.
How does inositol help with PCOS symptoms like irregular periods and fertility?
Inositol improves how your cells respond to insulin, which can lower insulin levels and stabilise hormones that control your cycle. Studies show that myo‑inositol and D‑chiro‑inositol can support egg maturation, improve ovulation rates and increase chances of pregnancy in women with PCOS. Over time, inositol may also reduce androgens and increase SHBG, which helps regulate cycles further. AusClin dietitians can design a nutrition plan that enhances these effects and supports your fertility goals.
Can I take inositol and metformin together for PCOS?
Yes, inositol and metformin are sometimes used together, as they can have complementary effects on insulin resistance and ovulation. However, combining them may increase the risk of low blood sugar or digestive side effects in some people. It’s important to discuss doses and timing with your GP or specialist and have your dietitian tailor your nutrition to minimise side effects. AusClin’s PCOS dietitians can coordinate with your medical team to safely integrate supplements and medications.
What type of inositol is best for PCOS, myo‑inositol or D‑chiro‑inositol?
Most PCOS research focuses on myo‑inositol alone or in combination with D‑chiro‑inositol, typically in a 40:1 ratio that mimics the body’s natural balance. Myo‑inositol supports insulin signalling and egg quality, while D‑chiro‑inositol appears more targeted to insulin and metabolic health. Too much D‑chiro‑inositol by itself may potentially impair egg quality in some women. An AusClin dietitian can help you choose evidence‑based formulations and avoid unbalanced products that don’t match current research.
How long does it take for inositol to work for PCOS?
Most clinical trials show meaningful changes in insulin and hormones after about 3 months of consistent inositol use, with some women noticing cycle changes sooner. Fertility‑related benefits, like improved ovulation and egg quality, often require 3–6 months. Results are stronger when inositol is combined with targeted diet and lifestyle changes, rather than used on its own. AusClin’s PCOS nutrition programs are typically structured around these time frames to track progress and adjust your plan.
Do I still need to change my diet if I’m taking inositol for PCOS?
Yes, diet and lifestyle changes still do most of the “heavy lifting” in PCOS, even if you’re taking inositol. Supplements can fine‑tune insulin and hormone balance, but they can’t fully override a pattern of eating that spikes blood sugar or doesn’t meet your nutrient needs. Research shows the best outcomes come when inositol is paired with balanced meals, adequate protein, fibre and movement. An AusClin PCOS dietitian can build an eating plan that makes your supplement work harder for you.
Is inositol safe to take long term for PCOS?
Current research and safety reviews suggest that inositol is generally well tolerated long term at typical doses used in PCOS studies. Side effects, when they occur, are usually mild digestive symptoms like nausea or loose stools. However, dosing and duration should be individualised, especially if you’re on other medications, trying to conceive, or have conditions like diabetes. AusClin dietitians can review your full health picture and liaise with your doctor to ensure safe, appropriate use.
Can inositol help with PCOS weight loss and cholesterol?
Studies show that inositol can lead to modest improvements in weight, LDL cholesterol and triglycerides, especially when combined with lifestyle change. It does this mainly by improving insulin sensitivity, which reduces fat storage signals and supports better metabolic health. However, it’s not a standalone weight‑loss solution and works best alongside tailored nutrition and movement. AusClin’s PCOS dietitians focus on sustainable, non‑restrictive strategies that target insulin resistance and cholesterol while protecting your relationship with food.
Do I need to see a dietitian if I’m already taking metformin or inositol for PCOS?
Seeing a dietitian is still highly beneficial, because medication or supplements alone rarely address all PCOS drivers. A PCOS‑skilled dietitian can help stabilise blood sugars, reduce cravings, manage GI side effects from metformin, and optimise nutrients that support hormones and fertility. They also help you interpret conflicting online advice and adapt your eating plan to your lifestyle, culture and symptoms. AusClin offers specialised PCOS nutrition consults to integrate your meds, supplements and diet into one coherent plan.
How can an Accredited Practising Dietitian help manage my PCOS at AusClin?
An Accredited Practising Dietitian at AusClin will first assess your symptoms, blood tests, medications and current eating patterns. They then create an evidence‑based nutrition plan targeting insulin resistance, hormone balance, cycle regularity and long‑term health risks like diabetes and heart disease. If you’re using inositol or metformin, they’ll help with dosing timing around meals, side‑effect management and realistic behaviour changes. Ongoing reviews track your cycles, lab results and symptoms so your plan can be adjusted as your body responds.
