Why Women Are More Prone to Iron Deficiency
Persistent fatigue, shortness of breath, difficulty concentrating? these symptoms are common in busy women, but they are not always “just stress.” Low iron is one of the most frequent underlying causes.
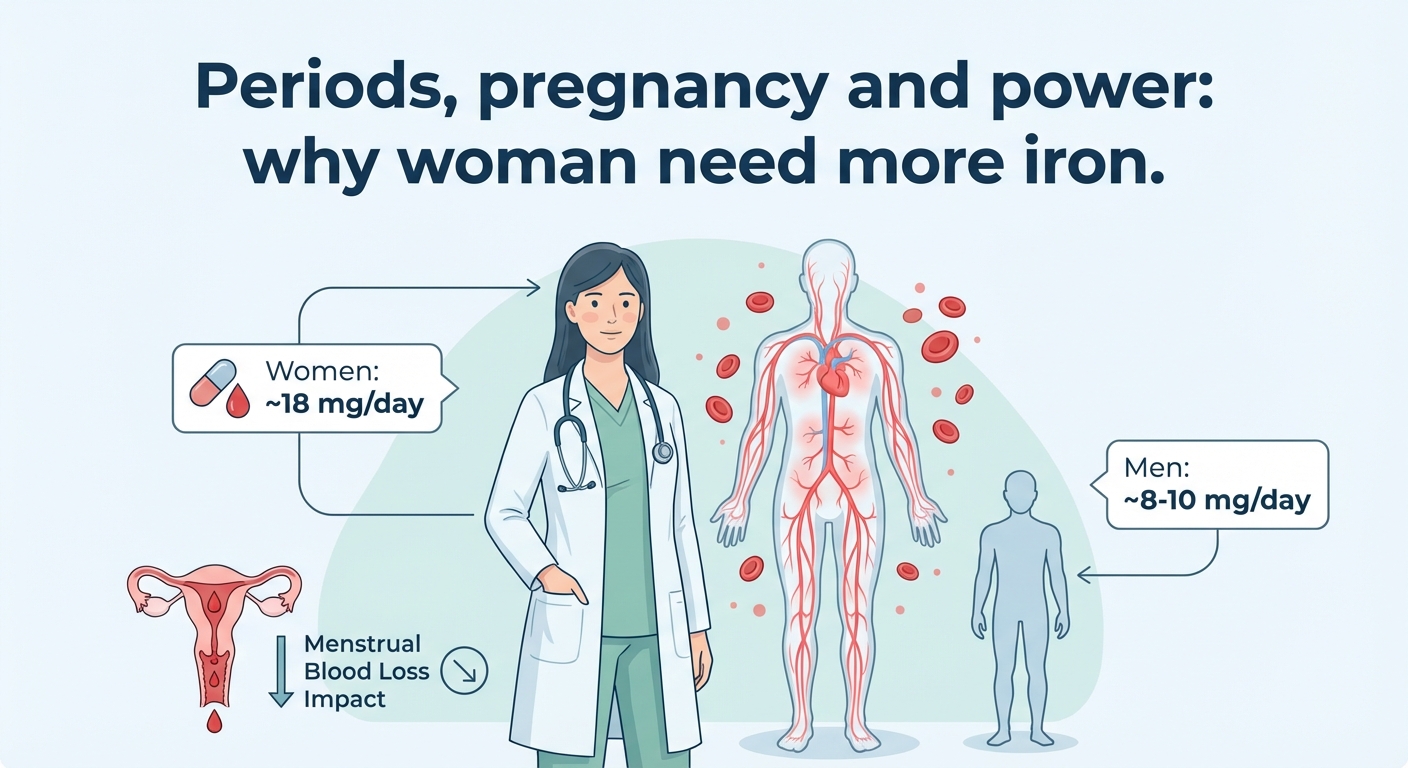
Women generally require around 18 mg of iron per day, compared with approximately 8 mg per day for men. The primary reason is menstruation. Monthly blood loss also means monthly iron loss, and over time this can gradually deplete iron stores if not adequately replaced through diet or supplementation.
This topic was recently highlighted in a professional women’s health webinar I attended, which reinforced how frequently low ferritin is overlooked in women presenting with fatigue, heavy menstrual bleeding, or difficulty conceiving. Iron deficiency remains one of the most common and most under-recognised nutritional concerns in women of reproductive age.
Understanding Ferritin: Your Iron Reserve
Ferritin is a protein that stores iron in the body. It functions as your internal iron reserve.
When ferritin levels fall, it indicates that iron stores are becoming depleted often before haemoglobin levels drop or anaemia develops. This makes ferritin a valuable early marker for identifying deficiency.
Women are particularly vulnerable to low ferritin due to:
-
Regular menstrual blood loss
-
Heavy or prolonged periods
-
Pregnancy and breastfeeding
-
Vegetarian or vegan dietary patterns
-
Closely spaced pregnancies
-
Certain gynaecological conditions
Low ferritin can cause symptoms even when standard blood counts appear “normal.”
Common Symptoms of Iron Deficiency
Iron deficiency often develops gradually, which is why it can go unnoticed for months.
Symptoms may include:
-
Ongoing fatigue
-
Reduced exercise tolerance
-
Shortness of breath with mild exertion
-
Dizziness or headaches
-
Pale or dry skin
-
Poor concentration
-
Feeling unusually cold
-
Heart palpitations
-
Restless legs
If untreated, iron deficiency can progress to iron deficiency anaemia, where the body cannot produce enough healthy red blood cells to transport oxygen effectively. This can significantly impact quality of life and daily functioning.
Because these symptoms overlap with other conditions, proper testing is essential before starting supplements.
When Should Iron Levels Be Tested?
A simple blood test through your GP can assess:
-
Haemoglobin
-
Ferritin
-
Other iron markers if indicated
Testing is particularly important for:
-
Women with heavy or painful periods
-
Those planning pregnancy
-
Women who are pregnant
-
Women experiencing unexplained fatigue
-
Vegetarians and vegans
-
Women with a history of iron deficiency
Early testing allows intervention before anaemia develops.
Iron Needs During Pregnancy
Iron requirements increase substantially during pregnancy.
Across the course of pregnancy, total additional iron requirements are estimated at 1,000–1,200 mg, including:
-
Approximately 500 mg for expansion of maternal red blood cells
-
Around 300 mg for the fetus and placenta
-
About 200 mg to account for blood loss during delivery
Meeting these increased demands through diet alone can be challenging, especially if iron stores were already low before conception.
Iron deficiency during pregnancy is associated with:
-
Increased maternal fatigue
-
Higher infection risk
-
Premature birth
-
Low birth weight
Routine antenatal blood tests help monitor iron status so that deficiency can be treated early and safely.
Haem Iron and Non-Haem Iron: Food Sources That Matter
Iron from food comes in two forms.
Haem Iron (More Easily Absorbed)
Found in animal-based foods:
-
Red meat (beef and lamb)
-
Poultry
-
Fish
-
Oysters and mussels
Haem iron is more readily absorbed by the body.
Non-Haem Iron (Plant-Based Sources)
Found in:
-
Lentils and beans
-
Tofu
-
Spinach
-
Nuts and seeds
-
Fortified cereals
Non-haem iron is less easily absorbed, but absorption can be improved through dietary strategies.
To Improve Iron Absorption:
-
Combine plant-based iron sources with vitamin C-rich foods (citrus, berries, capsicum, tomatoes)
-
Avoid tea and coffee with iron-rich meals
-
Separate calcium supplements from iron intake where possible
Thoughtful meal planning is especially important for women following plant-based diets.
Can You Have Too Much Iron?
While iron deficiency is common in women, excessive supplementation can cause problems.
High iron intake from supplements may lead to:
-
Nausea
-
Constipation
-
Abdominal discomfort
In rare cases, excessive iron can contribute to organ damage. Some individuals have genetic conditions such as haemochromatosis, which cause increased iron absorption.
For this reason, iron supplements should only be used under medical guidance following confirmed deficiency.
Supporting Iron Balance Across the Reproductive Years
Iron requirements fluctuate across life stages, particularly during puberty, the menstrual years, pregnancy, and postpartum recovery.
Maintaining healthy iron levels involves:
-
Eating a varied diet that includes iron-rich foods
-
Supporting absorption through smart food pairings
-
Monitoring symptoms
-
Testing when clinically indicated
Iron deficiency is common, but it is also highly treatable when identified early.
If you are experiencing persistent fatigue, heavy periods, or planning pregnancy, discussing iron testing with your GP is a sensible first step. Monitoring ferritin levels and addressing deficiency proactively can support energy, fertility, pregnancy outcomes, and long-term health.


Frequently Asked Questions
Why do women need more iron than men?
Women generally need around 18 mg of iron per day compared to about 8–10 mg for men because they lose blood (and therefore iron) every month during their periods. On top of that, pregnancy dramatically increases iron needs to support the baby, placenta and the mother’s increased blood volume. Without replacing this iron through diet or supplements, women are more likely to become iron deficient.
How much iron do I need during pregnancy?
Across an entire pregnancy, your body uses roughly 1,000–1,200 mg of extra iron to support your growing baby, placenta and the increase in your own blood volume. This is far more than usual daily needs and is difficult to meet from food alone, especially if your iron stores were low before conception. That’s why many pregnant women need careful monitoring and sometimes supplementation under the guidance of a healthcare provider or specialist nutrition service like AusClin.
What are the symptoms of low iron or iron deficiency in women?
Common symptoms of iron deficiency include constant tiredness, shortness of breath, reduced exercise tolerance, dizziness, poor concentration and pale skin. Some women also notice headaches, restless legs, hair shedding or feeling cold more often. These symptoms can appear even before full anaemia develops, especially when ferritin (iron stores) is low.
What is ferritin and why is it important for women?
Ferritin is a protein that stores iron in your body and releases it when needed, a bit like an iron ‘reserve tank’. When ferritin levels drop, it means your iron stores are low, often before your haemoglobin falls or anaemia shows up on standard tests. Women are particularly at risk of low ferritin because of periods, pregnancy and, in some cases, low-iron or plant-based diets.
When should I get my iron or ferritin levels checked?
It’s worth asking for a blood test that includes ferritin if you feel unusually tired, weak, breathless, or notice poor concentration or frequent headaches. Testing is especially important if you have heavy periods, follow a vegetarian or vegan diet, are planning a pregnancy, or are already pregnant. Early testing can catch low iron stores before they progress to anaemia and allow targeted treatment or nutrition support, such as AusClin’s fertility and preconception nutrition services.
What’s the difference between haem iron and non-haem iron?
Haem iron comes from animal foods like red meat, poultry, oysters and mussels, and is absorbed more efficiently by the body. Non-haem iron is found in plant foods such as beans, lentils, tofu, spinach and fortified cereals, but is less easily absorbed and more affected by other foods eaten at the same time. Women relying mostly on non-haem iron may need to be more strategic with their diet or consider supplements under professional guidance.
What are the best iron-rich foods for women?
The richest sources of highly absorbable haem iron include red meat, liver (within safe pregnancy limits), chicken, fish, oysters and mussels. Non-haem iron sources include legumes, leafy green vegetables, nuts, seeds, whole grains and iron-fortified cereals. Pairing these foods with vitamin C-rich options (like citrus, berries, capsicum) can significantly improve iron absorption.
How can I improve my iron levels without taking supplements?
You can increase iron intake by including haem iron sources such as lean red meat, poultry, oysters or mussels several times per week if you eat animal products. If you’re vegetarian or vegan, focus on iron-rich plant foods (legumes, tofu, leafy greens, fortified cereals) and always pair them with vitamin C sources while limiting tea and coffee around meals. Structured support from a nutrition-focused clinic like AusClin can help design a tailored meal plan that fits your preferences and health needs.
Can low iron affect pregnancy or fertility?
Yes, low iron and low ferritin before or during pregnancy can affect both maternal wellbeing and pregnancy outcomes. In pregnancy, iron deficiency is linked with increased risks of fatigue, infection, premature birth and low birth weight. Optimising iron status before conception through diet, blood testing and, if needed, supplementation is a key part of fertility and preconception care, which AusClin specifically supports.
Should I see a specialist like AusClin for low iron or preconception nutrition?
Seeing a specialist clinic can be very helpful if you have recurrent low iron, heavy periods, follow a restricted diet, or are planning a pregnancy. AusClin’s fertility and preconception nutrition services can review your blood tests, assess your diet, and create a personalised plan to optimise iron and other key nutrients. This proactive approach can improve energy, reduce deficiency risk and support healthier pregnancy outcomes.
